Hydrocephalus Nursing Intervention: Comprehensive Patient Care Guide
Hydrocephalus is a neurological condition characterised by an abnormal accumulation of cerebrospinal fluid (CSF) within the brain’s ventricles, leading to increased intracranial pressure. Effective nursing intervention plays a vital role in early detection, ongoing management, post-operative recovery, and long-term patient care.
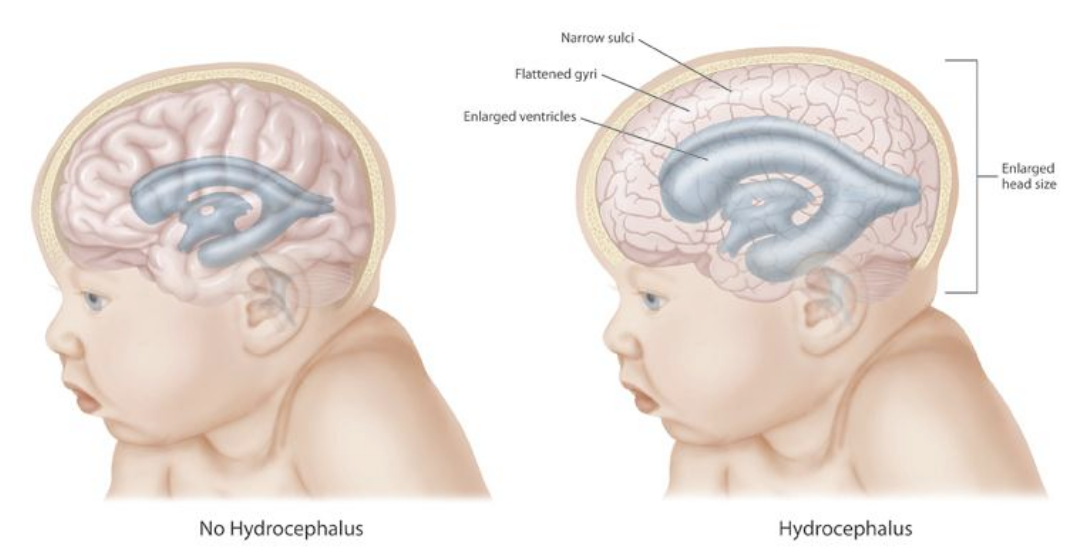
Understanding Hydrocephalus
Hydrocephalus may be congenital or acquired and can occur in infants, children, adults, or elderly patients. The condition results from an imbalance between cerebrospinal fluid production and absorption or obstruction in its flow.
If untreated, increased intracranial pressure can cause brain damage, neurological deficits, and life-threatening complications. Nursing professionals play a key role in recognising early signs and ensuring timely intervention.
Key Objectives of Nursing Intervention in Hydrocephalus
- Monitor neurological status and detect early deterioration
- Maintain optimal intracranial pressure
- Prevent infection and shunt-related complications
- Support recovery after surgical intervention
- Educate patients and caregivers for long-term management
Neurological Assessment and Monitoring
Continuous neurological assessment is the cornerstone of hydrocephalus nursing intervention. Nurses closely observe changes in consciousness, orientation, behaviour, pupil size, motor function, and vital signs.
- Persistent headache or vomiting
- Decreased level of consciousness
- Visual disturbances
- Seizures
- Bulging fontanelle in infants
Positioning and Intracranial Pressure Management
Proper positioning helps promote venous drainage and reduce intracranial pressure. Patients are usually nursed with the head elevated unless contraindicated. Sudden movements and activities that increase intracranial pressure should be avoided.
Nursing Care for Patients with Ventriculoperitoneal Shunts
Many patients with hydrocephalus undergo ventriculoperitoneal (VP) shunt placement to divert excess CSF. Nursing care is critical in preventing shunt malfunction and infection.
- Observe the shunt site for redness, swelling, or discharge
- Monitor for fever or signs of systemic infection
- Assess abdominal symptoms related to distal shunt placement
- Ensure strict aseptic technique during wound care
Post-Operative Nursing Care
After surgical intervention, patients require close monitoring in the immediate post-operative period. Nurses assess neurological recovery, pain levels, wound healing, and overall stability.
Patient and Family Education
Education is a vital component of hydrocephalus nursing intervention. Patients and caregivers must understand how to recognise warning signs that require urgent medical evaluation.
Long-Term Nursing Management
Hydrocephalus often requires lifelong follow-up. Nursing professionals assist in coordinating care, encouraging adherence to follow-up visits, and supporting rehabilitation when needed.
Frequently Asked Questions
Is hydrocephalus always treated surgically?
Not all cases require surgery immediately. The treatment approach depends on the cause, severity, and progression of symptoms.
What are the most important nursing priorities?
Neurological monitoring, infection prevention, patient education, and early detection of complications are the key priorities.
Can patients with shunts live normal lives?
With proper care, monitoring, and follow-up, many patients with shunts lead active and fulfilling lives.
