Surgical Intervention of Hydrocephalus: Procedures, Indications and Recovery
Hydrocephalus is a neurological condition in which excess cerebrospinal fluid (CSF) accumulates within the brain. As a result, intracranial pressure increases and begins to affect normal brain function. When conservative treatment no longer controls the condition or symptoms continue to progress, surgical intervention becomes necessary to relieve pressure and protect the brain from permanent damage.
Understanding Hydrocephalus
Hydrocephalus develops when the balance between CSF production and absorption becomes disrupted or when an obstruction blocks normal fluid flow. Consequently, cerebrospinal fluid accumulates inside the brain ventricles, causing them to enlarge and exert pressure on surrounding brain tissue.
This condition may be congenital or acquired and can affect infants, children, and adults alike. Without timely treatment, hydrocephalus can lead to cognitive decline, neurological deficits, and in severe cases, life-threatening complications.
When Is Surgical Intervention Required?
Doctors recommend surgical intervention of hydrocephalus when symptoms worsen or imaging shows progressive ventricular enlargement. In such cases, delaying treatment may increase the risk of permanent neurological damage.
- Persistent or worsening headache accompanied by vomiting
- Visual disturbances, seizures, or altered consciousness
- Increasing head size or bulging fontanelle in infants
- Progressive neurological or developmental decline
- Failure to respond to conservative medical management
Common Surgical Procedures for Hydrocephalus
Surgeons use several well-established techniques to treat hydrocephalus. However, the choice of procedure depends on the patient’s age, the underlying cause, and specific anatomical considerations.
Ventriculoperitoneal (VP) Shunt Surgery
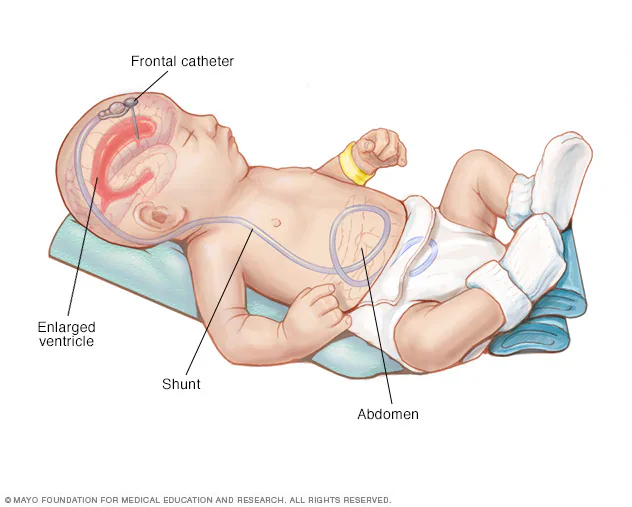
Ventriculoperitoneal shunt surgery remains the most frequently performed procedure for hydrocephalus. During this surgery, the surgeon places a shunt system that diverts excess CSF from the brain ventricles into the abdominal cavity, where the body safely absorbs it.
The shunt system includes a catheter, a pressure-regulating valve, and distal tubing. Together, these components maintain stable intracranial pressure and prevent further fluid accumulation.
Endoscopic Third Ventriculostomy (ETV)
Endoscopic third ventriculostomy is a minimally invasive option suitable for selected patients, particularly those with obstructive hydrocephalus. In this procedure, the surgeon creates a small opening in the floor of the third ventricle, allowing CSF to bypass the obstruction and flow normally.
Because ETV eliminates the need for a permanent shunt, it offers long-term benefits for appropriately selected patients.
Pre-Operative Evaluation
Before surgery, patients undergo detailed neurological examination along with imaging studies such as MRI or CT scans. These investigations help surgeons assess ventricular size, identify the cause of obstruction, and plan the most effective surgical strategy.
In addition, pre-operative counselling allows patients and caregivers to clearly understand the procedure, expected benefits, and potential risks.
Post-Operative Care and Monitoring
After surgical intervention, healthcare teams closely monitor patients for both clinical improvement and early signs of complications. During this period, doctors and nurses regularly assess neurological status, wound healing, and fluid balance.
As recovery progresses, careful observation ensures that shunt function remains adequate and that intracranial pressure stays within a safe range.
- Persistent headache, nausea, or vomiting
- Fever or redness along the shunt tract
- Drowsiness, confusion, or behavioural changes
- Seizures or sudden neurological deterioration
Recovery and Long-Term Follow-Up
Recovery following hydrocephalus surgery varies depending on age, cause, and symptom duration prior to treatment. Nevertheless, many patients experience noticeable improvement once intracranial pressure normalises.
Long-term follow-up remains essential, especially for patients with shunts, since adjustments or revision procedures may be required over time.
Risks and Complications
Although surgical intervention of hydrocephalus is generally safe, potential risks include infection, shunt blockage, over-drainage, or bleeding. Fortunately, early detection and prompt management significantly reduce long-term complications.
Frequently Asked Questions
Is hydrocephalus surgery a permanent solution?
Some patients require lifelong shunt support, while others treated with ETV may not need further intervention. Ultimately, outcomes depend on the underlying cause and individual response to treatment.
How long does recovery take?
Initial recovery usually takes a few weeks; however, neurological improvement may continue for several months with proper follow-up and rehabilitation.
Can hydrocephalus return after surgery?
Yes, recurrence or shunt malfunction can occur. Therefore, regular monitoring and follow-up appointments are critical for long-term safety.
